The tutorial content material on this publish, elaborated in collaboration with Bromatech, was independently developed and authorised by the GMFH publishing workforce and editorial board.
Getting recognized with IBS
The usage of symptom-based standards for the analysis of gastrointestinal practical problems could assist physicians to diagnose and legitimize such problems, and never be seen solely as a mixture of signs. A significant enchancment towards the understanding of those problems was launched by the factors of the Rome Basis. Many standards have been adopted and the final ones are associated to the Rome IV standards (2016). Rome IV modified the terminology from practical problems to problems of gut-brain interplay (DGBI) for the reason that time period “practical” implied illegitimacy and stigmatized the patients1.
Regardless that a analysis could possibly be made with the talked about standards, sure examinations could also be useful to exclude not solely inflammatory bowel illnesses and celiac illness, but in addition bile acid diarrhea, congenital sucrose-isomaltase deficiency, histamine mediated problems, systemic nickel allergy and excessive stool burden associated to pelvic ground dysfunction3. It has additionally been described that post-infective IBS and will happen in roughly 11% of individuals struggling an acute infection4. Current research additionally confirmed that COVID-19 would possibly enhance the chance of growing power intestinal signs and IBS5,6.
Many sufferers recognized with IBS may additionally search for additional analysis. Nevertheless, when physicians establish sufferers’ complaints as factual and may make a analysis based mostly on these standards, offering empathy, partaking the affected person in patient-centered interplay by describing the mechanisms of the dysfunction and by discovering doable options to enhance the physiological situation, these sufferers usually tend to settle for the analysis.
When the sickness turns into simpler to grasp, it’s also handled extra appropriately! The excellent news is that the constructive analysis of IBS utilizing symptom-based standards and restricted investigation is sturdy and secure, highlighting that IBS isn’t related to the event of natural gastrointestinal disease2.
IBS subtypes and overlapping signs affect their administration in medical observe
IBS is classed into 4 subtypes based mostly on predominant bowel habits:
IBS with predominant constipation
IBS with predominant diarrhea
IBS with blended bowel habits
IBS unclassified
Furthermore, there may be practical diarrhea and constipation when these signs are usually not related to ache. Practical stomach bloating and distension are recognized provided that these are the predominant signs and neither is required to make the analysis of IBS.
To fulfill the diagnostic standards of IBS in line with Rome IV, the next signs should be current: stomach ache, on common a minimum of 1 day every week previously 3 months (with the primary onset a minimum of 6 months earlier than analysis), related to two of the next signs: ache associated to defecation, change in frequency of stool or change in type (look) of stool1.
Focusing on the intestine microbiota to enhance IBS signs
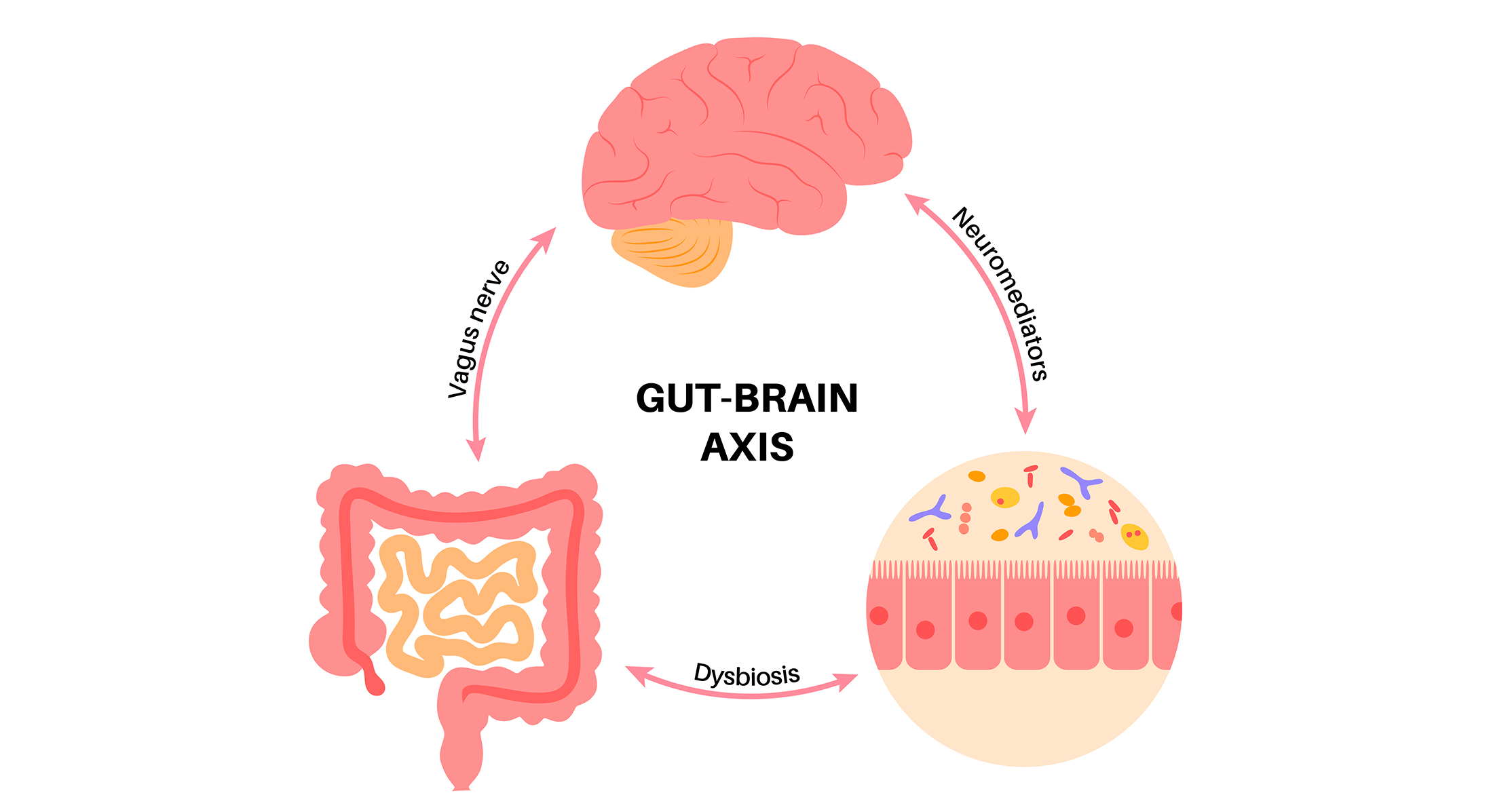
Though the etiology of IBS stays partially unknown, understanding the potential mechanisms has progressed quickly through the years involving the intestine microbiota, the gut-brain axis, the altered intestinal motility, the epithelial barrier, the immune system, the enteric nervous system, sure meals antigens, and psychological and genetic factors7.
The post-infective IBS mannequin reveals the central position of an alteration of intestine microbiota as a number one mechanism for IBS. Different medical eventualities linking IBS to intestine microbiota embrace the elevated danger of IBS induced by systemic antibiotics and IBS symptom enchancment after taking probiotics or non-absorbable antibiotics.
Microbiota dysbiosis in IBS has been acknowledged by the Rome Basis as a believable issue contributing to the disorder8. Experiments with animal fashions, aimed to point the significance and doable etiological position of the microbiota in IBS, have confirmed that the colonization of germ-free animals with microbiota from IBS sufferers can induce visceral hypersensitivity, impair intestinal permeability, and alter gastrointestinal transit time9.
Particular micro organism (e.g., a lower in Bifidobacterium and Faecalibacterium genus and a rise in Lactobacillaceae household, Bacteroides genus and Enterobacteriaceae household) have been related to the intestine microbiomes of sufferers with IBS, though it’s too early to find out if these microbes are a product or reason for IBS10. Additionally it is attention-grabbing to notice that IBS signs severity is expounded to particular traits of intestine microbiota composition (i.e., low microbial richness and Bacteroides enterotype enriched) and performance (i.e., low methane exhaled), which highlights the potential of modulating intestine microbiota as means to enhance IBS signs and the standard of life of those sufferers.
The involvement of the intestine microenvironment in IBS signs has led to the publication of a variety of research that recommend antibiotics, prebiotics and prebiotics could exert their therapeutic exercise by way of their influence on the degree of intestine microbiota composition, microbial metabolism merchandise (e.g., short-chain fatty acids) and intestine barrier integrity. Nevertheless, the usage of these intestine microbiome-based therapies isn’t all the time universally authorised. That is the case of rifaximin as non-absorbable antibiotic for IBS as its use is predicated on a possible capability of adjusting an altered intestine microbiota however extra medical research are wanted to raised set up our understanding on the therapeutic position of antibiotics in IBS11.
Future microbiome therapeutics within the pipeline for IBS embrace fecal microbiota transplants, microbial consortia, phages and engineered micro organism, whereas these methods are nonetheless beneath examine to translate their physiological results right into a doable medical observe. As an illustration, Quigley and colleagues just lately discovered the following era probiotic Blautia hydrogenotrophica (MRx1234) is a brand new potential secure therapeutic choice for sufferers with IBS-constipation, IBD-D or those that have blended symptoms12.
Current research additionally help different novel targets of potential curiosity for managing IBS signs. Histamine produced by particular intestine micro organism has been concerned in stomach ache, which suggests the position of concentrating on bacterial histamine for managing stomach ache in IBS. Additionally, following a low FODMAP eating regimen was superior to the spasmolytic agent otilonium bromide in bettering signs in sufferers with IBS in major care. Sequestering dangerous molecules within the intestine setting by way of an intestinal adsorbent has additionally proven promising in bettering stool consistency, stomach ache, stool frequency and urgency in sufferers with IBD-predominant diarrhea. General, these findings recommend the potential of impacting intestine microbiota and metabolites as technique of bettering IBS symptoms13.
Take-home messages
The usage of symptom-based standards for IBS helps physicians to make a analysis with restricted investigations.
Sure examinations could also be useful as a help to exclude much less widespread natural illnesses.
IBS can have a slow-onset or a rapid-onset which is usually associated to infections (post-infective IBS).
An altered intestine microbiota composition and performance seems to be concerned in IBS onset and growth, with particular intestine microbiota profiles associated to the severity of IBS signs.
Future microbiome therapeutics within the pipeline for IBS embrace fecal microbiota transplants, microbial consortia, phages and engineered micro organism, whereas are usually not prepared but to make use of within the medical observe.
References:
Drossman DA. Practical Gastrointestinal Issues: Historical past, Pathophysiology, Medical Options and Rome IV. Gastroenterology. 2016 Feb 19:S0016-5085(16)00223-7. doi: 10.1053/j.gastro.2016.02.032. Epub forward of print.
Khasawneh M, Craig OF, Gracie DJ, et al. A analysis of irritable bowel syndrome utilizing Rome IV standards and restricted investigations is sturdy in secondary care. Clin Gastroenterol Hepatol. 2023 Jun 9:S1542-3565(23)00444-5. doi: 10.1016/j.cgh.2023.05.022. On-line forward of print.
Camilleri M, Boeckxstaens G. Irritable bowel syndrome: therapy based mostly on pathophysiology and biomarkers. Intestine. 2023 Mar;72(3):590-599. doi: 10.1136/gutjnl-2022-328515.
Barbara G, Grover M, Bercik P, et al. Rome Basis Working Staff Report on Publish-An infection Irritable Bowel Syndrome. Gastroenterology. 2019 Jan;156(1):46-58.e7. doi: 10.1053/j.gastro.2018.07.011.
Marasco G, Cremon C, Barbaro MR, et al.; GI-COVID19 examine group. Publish COVID-19 irritable bowel syndrome. Intestine. 2022 Dec 9:gutjnl-2022-328483. doi: 10.1136/gutjnl-2022-328483. Epub forward of print.
Noviello D, Costantino A, Muscatello A, et al. Practical gastrointestinal and somatoform signs 5 months after SARS-CoV-2 an infection: A managed cohort examine. Neurogastroenterol Motil. 2022 Feb;34(2):e14187. doi: 10.1111/nmo.14187.
Chey WD, Kurlander J, Eswaran S. Irritable bowel syndrome: a medical evaluation. JAMA. 2015 Mar 3;313(9):949-58. doi: 10.1001/jama.2015.0954.
Simrén M, Barbara G, Flint HJ, et al.; Rome Basis Committee. Intestinal microbiota in practical bowel problems: a Rome basis report. Intestine. 2013 Jan;62(1):159-76. doi: 10.1136/gutjnl-2012-302167.
Crouzet L, Gaultier E, Del’Homme C, Cartier C, Delmas E, Dapoigny M, Fioramonti J, Bernalier-Donadille A. The hypersensitivity to colonic distension of IBS sufferers will be transferred to rats by way of their fecal microbiota. Neurogastroenterol Motil. 2013 Apr;25(4):e272-82. doi: 10.1111/nmo.12103.
Pittayanon R, Lau JT, Yuan Y, et al. Intestine Microbiota in Sufferers With Irritable Bowel Syndrome-A Systematic Evaluation. Gastroenterology. 2019 Jul;157(1):97-108. doi: 10.1053/j.gastro.2019.03.049.
Iribarren C, Maasfeh L, Öhman L, et al. Modulating the intestine microenvironment as a therapy technique for irritable bowel syndrome: a story evaluation. Intestine Microbiome. 2022; 3:e7. doi: 10.1017/gmb.2022.6.
Quigley EMM, Markinson L, Stevenson A, et al. Randomised medical trial: efficacy and security of the stay biotherapeutic product MRx1234 in sufferers with irritable bowel syndrome. Aliment Pharmacol Ther. 2023; 57(1):81-93. doi: 10.1111/apt.17310.
Simrén M. Focusing on the intestine microenvironment in IBS to enhance signs. Nat Rev Gastroenterol Hepatol. 2023; 20(2):69-70. doi: 10.1038/s41575-022-00718-3.