The academic content material on this publish, elaborated in collaboration with Bromatech, was independently developed and permitted by the GMFH publishing group and editorial board.
As soon as considered sterile, the bladder accommodates microbes that might affect well being
These days, it’s fairly fascinating to see how omics sciences are advancing our information; the molecular strategies of genomics, metagenomics, and proteomics can exactly decide the composition and variety of the microbial communities which are current in numerous anatomical websites and may determine metabolites which are produced by microorganisms positioned there.
Thus, research on this regard are progressively and quickly growing, and consequently, physique websites such because the bladder, which had been erroneously thought of sterile till a number of years in the past, at the moment are seen in a different way. Furthermore, earlier than metagenomics was launched, urine samples had been studied utilizing commonplace strategies based mostly on tradition in media that allowed the expansion of a restricted variety of micro organism, resembling Escherichia coli, whereas shedding the potential of highlighting the presence of different species.
Right this moment, we all know that kidneys, the urinary tract, the bladder, the endometrium, and even ovaries host their very own peculiar microbiota [1]. In actual fact, it’s presently accepted not solely that wholesome topics stably host a microbiota within the urinary tract, but in addition that this microbiota differs from topics with urogenital problems [2-7]. Nevertheless, as with different human physique samples with low biomass microbiome, resembling breast milk, the variability of strategies for urine assortment, processing, and evaluation could result in conflicting outcomes between research in regards to the urinary microbiome.
The gut-bladder axis emerges as one other dimension of microbiome well being
Urogenital infections have an effect on multiple in two ladies, and over 10% of those sufferers change into carriers of antibiotic-resistant bacterial strains [8,9]. The intestine microbiota is a reservoir for uropathogenic micro organism resembling E. coli, whereas its precise function in urinary tract infections (UTIs) is unknown. Thus, a shift in how we conceptualize the connection between urogenital and intestine microbiota is obligatory.
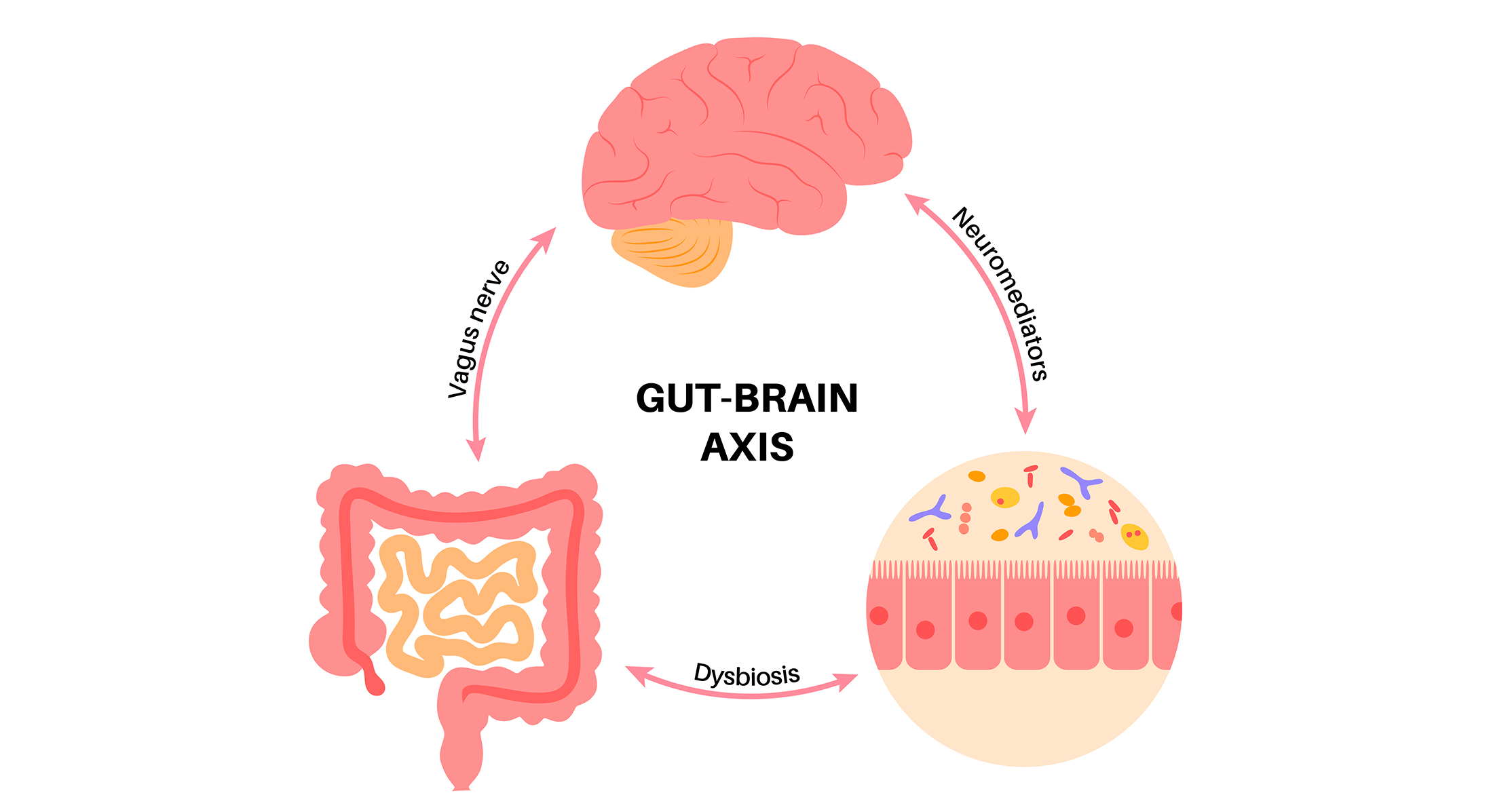
The organic and microbiological methods of varied organs are speaking constantly via connection networks that play a elementary function in sustaining homeostasis [10]. We’re used to contemplate solely the communication between two organs once we discuss “axis” (e.g. gut-urogenital axis, gut-brain axis, and so forth.).
Nevertheless, that is an oversimplification of a fancy relationship between the host and its microbiota, which isn’t restricted to the dialogue between two distinct organic locations or axes. It consistently and concurrently entails your complete host-microbiota ecosystem; direct and oblique indicators ubiquitously exchanged through chemical transmitters, neural pathways, and the immune system [11].
By conserving in thoughts the advanced and mutual affect between ecosystems, it’s elementary to grasp the significance and impression that intestine dysbiosis could have on vaginal and urinary ecosystems and vice versa. That is essential to make clear the pathophysiology of urogenital illnesses and, subsequently, goal each analysis and affected person care.
From bench to bedside: rising interventions focusing on the gut-bladder axis
It’s useful and needed to contemplate that the gastrointestinal system and its microbiota are intently speaking. As well as, this may increasingly assist us to grasp the genesis of scientific indicators and the onset and growth of signs. It has additionally been hypothesized that an imbalance within the urogenital-gut-brain axis, with a consequent dysregulation of the associated communication pathways, might decide a state of visceral hypersensitivity, amplified sensitivity, and hyperalgesia of the urogenital tract. This viewpoint would additionally clarify the advanced signs that come up in sufferers with relapsing and interstitial cystitis, who typically current an altered emotional/cognitive state, nervousness, temper deflection, and hypervigilance [12].
UTIs afflict an estimated 1 billion ladies annually. Whereas antimicrobial brokers are probably the most frequent therapeutic choice, they’re often accompanied by unwanted effects and secondary infections, which has prompted scientists to discover exogenous (together with oral) administration of lactobacilli in its place administration routine to antimicrobial therapy and prophylaxis [13]. From this attitude, the administration of particular strains of probiotics might play an more and more vital function in urogenital well being. [14, 15].
Contemplating probiotics as bioactives can also be vital as a result of this might permit physicians to cut back the prescription of antibiotics and consequently scale back antibiotic resistance. Different methods to stability the vaginal microbiome are presently being explored. They embody including probiotics to straightforward of care in bacterial vaginosis [16] and performing vaginal microbiome transplants [17].
In conclusion, rising proof suggests there’s a urinary microbiome that is likely to be concerned within the onset of UTIs. Whereas it stays to be seen whether or not there’s a secure urinary tract microbiome and its physiological relevance, interventions-such as probiotics or outlined fecal microbiota transplants-added to the present commonplace of care might assist individuals with UTIs who don’t reply to antibiotics.
References:
Zucko J, Melvan, Oros, Starcevic, et al. Present Viewpoint on Feminine urogenital Microbiome – The trigger or the consequence? Microganisms 10.3390/microrganisms 11051207 -2023
NIH HMP Working Group; Peterson, J.; Garges, S.; Giovanni, M.; McInnes, P.; Wang, L.; Schloss, J.A.; Bonazzi, V.; McEwen, J.E.; Wetterstrand, Ok.A.; et al. The NIH Human Microbiome Venture. Genome Res. 2009, 19, 2317–2323. [CrossRef] [PubMed]
Oros, D.; Ceprnja, M.; Zucko, J.; Cindric, M.; Hozic, A.; Skrlin, J.; Barisic, Ok.; Melvan, E.; Uroic, Ok.; Kos, B.; et al. Identification of Pathogens from Native Urine Samples by MALDI-TOF/TOF Tandem Mass Spectrometry. Clin. Proteom. 2020, 17, 25. [CrossRef] [PubMed]
Worth, T.Ok.; Dune, T.; Hilt, E.E.; Thomas-White, Ok.J.; Kliethermes, S.; Brincat, C.; Brubaker, L.; Wolfe, A.J.; Mueller, E.R.; Schreckenberger, P.C. The Medical Urine Tradition: Enhanced Methods Enhance Detection of Clinically Related Microorganisms. J. Clin. Microbiol. 2016, 54, 1216–1222. [CrossRef]
Brubaker, L.; Putonti, C.; Dong, Q.; Wolfe, A.J. The Human Urobiome. Mamm. Genome 2021, 32, 232–238. [CrossRef] [PubMed]
Marimuthu, A.; O’Meally, R.N.; Chaerkady, R.; Subbannayya, Y.; Nanjappa, V.; Kumar, P.; Kelkar, D.S.; Pinto, S.M.; Sharma, R.; Renuse, S.; et al. A Complete Map of the Human Urinary Proteome. J. Proteome Res. 2011, 10, 2734–2743. [CrossRef][PubMed]
Perez-Carrasco, V.; Soriano-Lerma, A.; Soriano, M.; Gutiérrez-Fernández, J.; Garcia-Salcedo, J.A. Urinary Microbiome: Yin and Yang of the Urinary Tract. Entrance. Cell. Infect. Microbiol. 2021, 11, 617002. [CrossRef]
Brubaker L, Wolfe AJ. Microbiota in 2016: associating infec- tion and incontinence with the feminine urinary microbiota. Nat Rev Urol 2017;14:72-4.
Leue C, Kruimel J, Vrijens D, Masclee A, van Os J, van Ko- everinge G. Purposeful urological problems: a sensitized defence response within the bladder-gut-brain axis. Nat Rev Urol 2017;14:153-63.
Cryan JF, O’Riordan KJ, Cowan CSM, Sandhu KV, Bastiaans- sen TFS, Boehme M, et al. The microbiota-gut-brain axis. Physiol Rev 2019;99:1877-2013.
Morais LH, Schreiber HL 4th, Mazmanian SK. The intestine microbiota-brain axis in behaviour and mind problems. Nat Rev Microbiol 2021;19:241-55.
Skender T, Ioannis Alexandros, L. Santacroce et al. An summary of the microbiota of the human urinary tract in well being and illness: present points and views. Life MDPI Urinary Microbiome and Genitourinary System Issues https://doi.org/10.3390/life13071486
Reig G. Probiotic Lactobacilli for urogenital well being in ladies. J Clin Gastroenterol. 2008; 42(Suppl 3 Pt 2):S234-6. doi: 10.1097/MCG.0b013e31817f1298.
Reid G, Bruce AW, Fraser N, et al. Oral probiotics can resolve urogenital infections. FEMS Immunol Med Microbiol. 2001; 30(1):49-52. doi: 10.1111/j.1574-695X.2001.tb01549.x.
Reid G. Perspective: microbial interventions within the urinary tract. Microbiome Res Rep. 2023; 2(1):3. doi: 10.20517/mrr.2022.17.
Cohen CR, Wierzbicki MR, French AL, et al. Randomized trial of Lactobacillus crispatus CTV-05 to stop recurrence of bacterial vaginosis. N Engl J Med. 2020; 382(20):1906-1915. doi: 10.1056/NEJMoa1915254.
Nationwide Library of Drugs. Vaginal Microbiota Transplant (MOTIF). Obtainable on: https://clinicaltrials.gov/research/NCT04046900
rnrnrnrnrnrnrnrnrn”,”physique”:””,”footer”:””},”superior”:{“header”:””,”physique”:””,”footer”:””}}”,”gdpr_scor”:”true”,”wp_lang”:”_en”};
/* ]]> */